Addiction Surgery: Is This the Future of Treatment?
Forget recovering addict. This new addiction surgery leaves you recovered – with no chance of relapse.
Or does it?
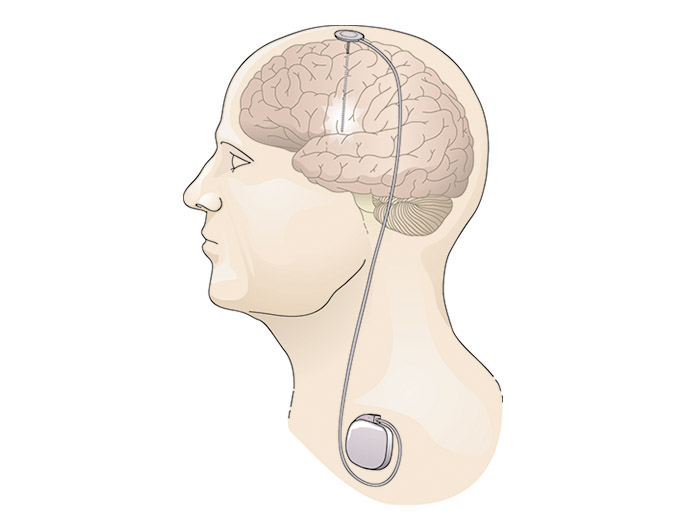
The procedure is called Deep Brain Stimulation (DBS). DBS is pretty much just what it sounds like: deep brain surgery. Only in this case it’s only minimally invasive. In fact, the surgeons are putting something into the head (an electrode) rather than taking something out. They’re also implanting a neurostimulator (aka a “brain pacemaker”) just below the collarbone. The device then sends electrical impulses to specific parts of the brain.
Before now, DBS targeted the parts that controlled movement. Consequently it was effective in treating disorders such as epilepsy and Parkinson’s disease. Now though docs are targeting the parts of the brain that control addiction.
Well they’ve done it once anyway. A year ago. And the patient remains drug-free.
Really.
Last Ditch Effort
The man’s name is Gerod Buckhalter. The 33-year-old has been battling opioid addiction for 18 years. That’s right. Buckhalter’s been addicted to opioids since the age of 15. He hasn’t been able to get clear of them either. No matter what he’s tried.
And Buchalter has apparently tried everything. More than thrice. Inpatient. Outpatient. M.A.T. Abstinence. Holistic. 12 Steps. Equine. You get the idea. The more he tried the harder it became. Why? Because every time Buckhalter went back to the treatment board, he was that much more addicted. Meaning his brain had further altered itself to fit its addiction.
It’s no wonder traditional treatment didn’t work. Band-aids don’t stop internal bleeding. And therapy can’t rewire the brain. Oh, complete abstinence will eventually reset the ol’ cranium. But that takes time. Lots of time.
What do you do in the meantime?
There are also a range of other issues, including geography, family and psychology. Lead doctor Ali Rezai addressed some of these issues with the BBC last year. Right before Buckhalter went in for his revolutionary addiction surgery.
“Addiction is complex,” said the good Doctor. “There are a range of social and genetic dynamics at play and some individuals will have a lack of access to treatments. So their brains will slowly change and they will have more cravings.”
In other words, there comes a point when there simply aren’t any more options. None. When even a combination of every trick in the book won’t suffice.
DBS is for those rare occasions.
“This treatment is for those who have failed every other treatment,” said Dr. Rezai, “whether that is medicine, behavioural therapy, social interventions. It is a very rigorous trial with oversight from ethicists and regulators and many other governing bodies.”
Again, the last ditch effort you take only after you’ve exhausted every other last ditch effort.
The Addiction Surgery
Buckhalter got the greenlight last year. First he was scanned. Then he was scanned and scanned again. Then surgeons made a small hole in his skull and inserted a tiny electrode into his brain. The electrode measured 1mm. It snapped right into the area of the brain that controls addiction and impulses.
A small battery was then placed in his collarbone. Then docs got busy monitoring Buckhalter’s brain activity. The charge is calibrated to effectively reduce his cravings. A little adjustment here. A slight adjustment there. And voila! Cravings reduced to zero.
One year later, Buckhalter remains clean and sober.
After 18 years of constant and continuous opioid addiction.
No foolin.’
“I was as bad as they can get,” said Buckhalter. “And if [DBS] can help me, it can help anybody.”
Not Your Grandma’s Cosmetic Surgery
Doc Rezai wants to be absolutely clear: Yes, DBS is a major breakthrough. In fact, it has the potential to change millions of people’s lives. But it should not be treated like some ordinary cosmetic procedure.
“I think it is very good for science and we need more science to advance the field and learn more about the brain,” the Doc told Good Morning America. Adding this represents a huge step in helping those overcome some of the biggest challenges they face.
Nevertheless:
“This is not for augmenting humans and that is very important. This is not a consumer technology.”
More importantly:
“When it comes to applications, [DBS] needs to be heavily regulated. This is not like getting a flu shot or a tattoo.”
Yes, DBS has helped hundreds pf thousands who are suffering from Parkinson’s. It’s also helped scores of people suffering from epilepsy and even OCD. Yet again:
“Surgery has inherent risks and is not trivial. It is only for those with chronic disease who have failed all other treatments and are without hope.”
Got it?
Healing Properties Says
Healing Properties applauds Dr. Ali Rezai, as well as the entire staff at West Virginia University Medicine Hospital. For their efforts of course. But also for their courage and empathy. Few medical professionals go out on a limb to help the addiction community. Even fewer go out to such great good degree. That they all did just that must make Hippocrates incredibly proud.
We also heed Dr. Rezai’s warning. And we echo his caution. Yes, Deep Brain Stimulation represents a breakthrough. It may even be a sign of great things to come. But it’s not a one-stop cure-all. So don’t run out and start pounding dope thinking this new addiction surgery will get you off the hook. It won’t. And it shouldn’t. DBS is for the most problematic of troublesome cases. The worst of the beyond hopeless. Please consider that.
It is however okay to be encouraged by the findings. And to applaud Gerod Buckhalter on his sobriety. We bet he’s thrilled after his first sober year in forever. And we wholeheartedly congratulate him. We also hope this is just the first of many sober years to come.
In fact we hope that everyone who needs help gets help. And that they don’t wait for some revolutionary addiction surgery either. Substance use disorder doesn’t get better. And it won’t go away simply by ignoring it. So please don’t sweep your addiction under the table.
Instead seek treatment. Make a call. The call. Change your life. Save your life. It’s worth saving. And so are you.
(Image courtesy of the National Institute of Health’s National Institute of Neurological Disorders and Stroke — with great gratitude.)